Imaging system enhances skin-cancer detection
Andrew Wilson, Editor, [email protected]
Founded in 1999, Biocam (Regensburg, Germany; www.biocam.de) introduced its first system for early skin-cancer detection in 2002. Dubbed Dyaderm, the turnkey system provides physicians with a method of determining whether specific tumors exist by capturing visible and fluorescent images of a patient’s skin.
To obtain these images, the patient’s skin is coated with a cream containing 5-aminolevulinic acid (5-ALA). This is metabolized by the body to heme (the color part of hemoglobin), producing the chemical protoporphyrin IX (PP-IX), a chemical that absorbs energy when subjected to illumination at a 405-nm blue wavelength. This energy is then transmitted from the body as red light. In cancer cells, however, the concentration of PP-IX is far higher than that of normal cells, so that the red light emitted from the cancerous region will be far higher than that emitted from normal skin tissue.
“By exploiting this fact,” says Gregor Liebsch, manager of imaging technology with Biocam, “the Dyaderm system can capture and display real-time color images of the skin and their corresponding fluorescence images. These also can be superimposed and pseudocolored to better highlight relevant parts of any tumor that may exist.” In the design of the system, a halogen-based strobe light source from Rapp OptoElectronic (Hamburg, Germany; www.rapp-opto.com) is triggered from a host PC to produce shorter-than 100-ms pulses along a liquid-filled light guide.
“By embedding the end of the light guide into the camera housing,” says Liebsch, “we focus the illumination directly above the area where the image needs to be acquired.” To capture both color and fluorescence images simultaneously, the system uses a modified version of the Pixelfly CCD camera system from PCO (Kelheim, Germany; www.pco.de). “Because the Pixelfly uses an ICX-414 CCD from Sony Electronics (Park Ridge, NJ, USA; www.sony.com/videocamera),” says Liebsch, “the camera can capture the 12-bit images required by the system.”
To digitize images from the camera, a PCI frame grabber (also from PCO) is used. “By coupling the TTL trigger from the light source to the input trigger of the frame-grabber board,” says Gerhard Holst, R&D manager at PCO, “the exposure time of the camera can be precisely synchronized with the light source.”
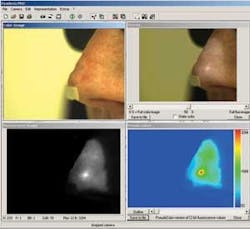
Because images must be captured in real time using both white and blue lighting conditions, the system is triggered to capture every fifth image under fluorescent light. In this way, both real-time color and fluorescence images are captured and transferred to the host PC memory. While color white-light-illuminated images can be directly transferred to the display after de-Bayering, fluorescence data from the color CCDs red pixels are extracted to produce a one-quarter VGA image.
“Because the red information, containing the relevant fluorescence signal, is one-quarter the size of the full-color image,” says Liebsch, “the image is then linearly interpolated to produce a full VGA image that can be displayed simultaneously with the white-light illuminated image.” After interpolation, both images can be superimposed to allow a physician to localize any fluorescence spots at the examined skin area.
With an end-user price of approximately €26,000, the Dyaderm system is currently in use in a number of university hospitals, mainly in Germany. According to Liebsch, Biocam is also developing a second-generation system that will integrate an LED source and camera and image-processing functions into a single hand-held system targeted for the endoscopy market.