Medical Imaging: Digital light projector localizes treatment of skin diseases
Skin diseases such as psoriasis are characterized by red patches that may vary in size and location on the body. To treat this disorder, the skin is exposed to ultraviolet (UV) light in a process known as phototherapy. This suppresses the immune system and reduces the inflammatory effects of the disease. Depending on whether UV treatment is performed in conjunction with drug therapy, two different wavelengths are used - UVA (with a spectrum of 320nm - 400nm) or UVB (with a spectrum of 300nm - 320nm).
"In the past," says Dr Friedrich Lüllau, President of Lüllau Engineering (Lüneburg, Germany; www.luellau-engineering.de), "phototherapy was administered to the entire body, with unaffected areas being covered to reduce the effects of skin cancer." Today, phototherapy systems such as the company's Skintrek system can be used to administer the UV light to a specific, localized area of the skin.
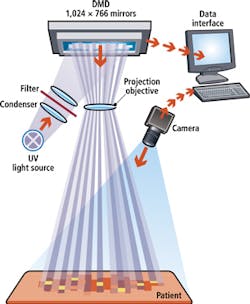
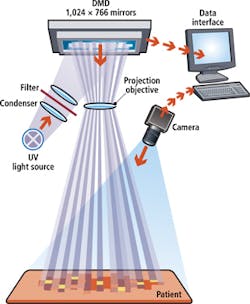
To localize the area to be exposed to UV radiation, the topography of the skin must first be computed. This is achieved by projecting a white light source onto a digital light projector (DLP) from Texas Instruments (Dallas, TX, USA; www.ti.com). This DLP modulates the white light and projects a two dimensional grid array across the body. Images of this grid are then captured by a custom-built camera and the data is processed and the contours of the lesions defined along their edges.
After this is accomplished, continuous rays from a UV-light source are bundled and filtered in such a way that either UVA or UVB rays are projected onto the DLP. The DLP then projects approximately 800,000 individual, controllable pixel-rays with a size of 0.14 mm x 0.14 mm onto the skin's surface. Required doses of UV energy are determined by the doctor and the topological information of the skin's surface. Once this is established, only the required pixel-rays on the DMD will be activated to treat the defined areas of skin.
Not only does this ensure that an accurate and precise dose of energy will be targeted to the affected areas but it allows the doctor to choose from multiple dosage profiles which, for example, can be lowered near the edge of a lesion.
Because topological data is collected in real-time, any movement of the patient will be registered by the camera allowing the UV-exposure to be automatically adjusted within fractions of a second. Thus, should the patient move, no healthy skin will be exposed to UV-rays. At present, the $130,000 system has been installed at multiple locations throughout Europe including the Charité University (Berlin, Germany; www.charite.de) where it is undergoing clinical trials. A video of the fully automated system in operation can be seen at http://bit.ly/1k2rFbj.
Vision Systems Articles Archives