Standards shape medical imaging
To meet overwhelming medical-imaging demands, workstation suppliers are building a standard infrastructure to handle patient data.
By Joe Hallett,Contributing Editor
The National Electrical Manufacturers Association (NEMA; Rosslyn, VA) interface standard dealing with the digitization of medical images—DICOM (Digital Image Communication)—was developed jointly with the American College of Radiology (ARC; Reston, VA) to facilitate interoperability of medical equipment used in Picture Archiving and Communications Systems (PACSs). A PACS aims at connecting imaging devices, or modalities, and other compatible peripherals with workstations, storage devices, and servers.
Says Michael Flynn, a medical physicist with the Henry Ford Health System (Detroit, MI), "DICOM has been the essential standard that allows equipment from various vendors to interconnect in a reasonable way. Four or five years ago, the only way to integrate was to go through standards converters, but their use is dwindling."
Medical imaging is no longer just about x-ray radiology. Says Flynn, "DICOM object definitions are set now for technologies such as MRI (magnetic resonance imaging), ultrasound, and CAT (computer-aided tomography). There is nothing pressing in these technologies, but the [DICOM] standard is being extended to include visible imagery for uses such as pathology, microscope images, patient photographs, and ophthalmology. There still are issues regarding image quality, particularly in the display environment."
Workstations from manufacturers such as GE Medical Systems and Siemens Medical Systems are used in high-volume radiology departments, where they are called clinical or diagnostic workstations, depending on the display. They are worklist driven, with macros giving one-button access to features for individual radiologists. High-end workstations are used for reading x-rays with high-quality 2 x 2.5-kpixel (monochrome) images on CRT-based displays. However, flat-panel displays are being introduced at clinical review workstations where space is at a premium and image quality is less critical but with the same functions and features. Color resolution is around 1100 x 800 pixels.
Filmless digital imaging is taking over in many new medical installations. Digital images are never misplaced, and multiple copies can be accessed simultaneously. The result is "a leap in image quality and throughput," according to Thomas Prenzno, a product manager for GE Medical Systems (Waukesha, WI). "With end-to-end digital capabilities all the way from capture to store, we see 85% to 90% direct digital capture compared to 5% to 8% scanned images from film."
However, suppliers of DICOM-compliant equipment must still consider their options. "The standards are complicated and are written in a strange syntax. It is expensive (to support DICOM in-house), and big companies have been slow to commit, according to Flynn. "Large companies can support standards committees, and they may have their own documents that help in understanding the standards. So there is an emerging business for consultants helping smaller businesses add DICOM compliance."
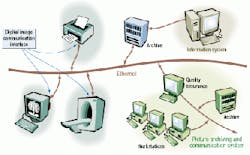
COMMUNICATION SYSTEMSA PACS typically consists of image-acquisition systems, servers with local storage, diagnostic and clinical workstations, archival storage, and information attachment functions (see figure above). Says Herman Oosterwijk, president of OTech Inc. (Aubrey, TX), a health-care technology consulting company, "All PACS use DICOM, but PACS are differentiated by features such as image management, open standards support, service, cost, and ease of connecting to the digital modalities [such as computed tomography and magnetic resonance]."Each DICOM object consists of a data file with a unique header, which comprises several thousand characters of header data in variable length fields, plus up to 10 to 20 Mbytes of storage for the image file. At its core are about 100 fields of data specific to the image that contain tags with patient and image information, such as view, date, and radiometry parameters. And there can be several hundred others, including 'shadow fields,' that are specific to particular instruments. Manufacturers also may include data for proprietary purposes.
Flynn says, "The patient's name must always be in a particular part of the DICOM header. And there also is a need to associate each image with other information in the hospital, such as doctors' reports, through index and accession numbers." Worklist management using DICOM avoids data-entry errors—estimated by some to be as high as 5%—by displaying a patient's name in a selection list.
Eric Pearce, a product manager for GE Medical Systems, agrees that whether clinical user or radiologist, each person expects to do business in a familiar way. "Our workstations are designed around high-volume radiology departments, where they're called clinical or diagnostic workstations, depending on the display. They are worklist driven, with macros giving one-button access to features for individual radiologists. High-end workstations are used for reading x-rays with high-quality 2 x 2.5-kpixel (monochrome) images on CRT-based displays (see images on p. 41). We're just introducing flat-panel displays (FPDs) at clinical review workstations—where space is at a premium and image quality is less critical—with the same functions and features. Resolution is around 1100 x 800 pixels (color). We treat nuclear medicine and ultrasound under the same umbrella as x-ray," he adds.
Otech's Oosterwijk says, "The user interfaces at the workstations are getting more and more alike, especially the Web-based viewers; they all use standard browsers. Another reason is that there are a couple of software companies, such as Cedara (Mississauga, Ont., Canada) and Applicare (Zeist, The Netherlands), that deliver viewers to many corporations. We do about a quarter-million exams per year. I can sit at one station and access any patient's lab data and notes that used to come from patient records."
Dr. Michael Pearson, assistant professor of Muscular Skeletal Radiology at Oregon Health Sciences University (OHSU; Portland, OR), sounds positive about his Agfa (Wilmington, MA) medical imaging system. "It's well integrated and seamless between patient medical records and images. I just pick an icon to view reports on PACS. Some hospitals are totally digital. Small hospitals may still be using film in ten years, but within 25 years, all images will be digital."
A medical physicist who does radiation calculations or quality assurance can become an organization's PACS radiology expert. But even in large hospitals, doctors have concerns about support for these new tools. "In a 150-bed hospital, a medical technician knows everything, but not in a big institution that puts millions of dollars into a system," adds Pearson. "We're all doing things together—doctors and systems people—to solve problems. But we have to depend on systems administration. The hospitals have to decide whether to buy extended warranties and service contracts."
SYSTEM SUPPLIERSPotential customers for PACS vary in size from small clinics to large hospitals. One measure of size is the number of x-ray exams performed. "More than 120,000/ year is big; 50,000 to 120,000/year is medium," says OTech's Oosterwijk. "Also, teaching and nonteaching institutions differ because the teaching hospitals have a different workflow and are typically not as production-oriented."Other medical-system suppliers, such as Philips (Shelton, CT) and Siemens (Concord, CA), offer complete turnkey PACSs to large hospitals and may engage in customizing solutions. Smaller institutions that can't afford the large systems can look to other avenues. Says Oosterwijk, whose firm specializes in connectivity, "They first ask their existing modality and film vendors, and then, a PACS vendor. Increasingly, there is a place for consultants."
Dynamic Healthcare Technologies (Lake Mary, FL) is a small firm that develops clinical software and radiology information systems and integrates DICOM-compliant equipment for smaller institutions. Marketing director Jim Mulvaney says, "Our PACS is Windows-NT-based using Compaq, IBM, or Hewlett-Packard computer equipment. It is fairly easy to capture images with DICOM scanners or conversion boxes. Servers are desktop PCs using a large RAID (random array of independent drives) storage facility from Storage Technology or IBM. The choice now for (archival) storage is between tape and optical, with price and reliability favoring tape for large 1- to 20-Tbyte storage units. Display is also taken care of, from simple PC monitors to diagnostic workstations to high-resolution monitors, and flat-panel displays keep getting better. They're okay for (clinical) viewing but need higher resolution and brightness for diagnostics."
A DICOM system requires TCP/IP, which supports communication protocols such as Ethernet for use with a variety of computer systems and speeds. "Several vendors push ATM [asynchronous transfer mode]," said Oosterwijk, "but Gigabit Ethernet seems to be the most efficient and cost-effective."
Distributing images through a hospital is handled well by servers with large, fast disks that can store and transmit easily over a switched 10- or 100-Mbit/s Ethernet. A T-1 line can be installed for linking to outside facilities, or, depending upon load, DSL or cable modems can be used, according to Mulvaney. "Even 56-kbit/s phone modems are okay for sending a few cases home at night."
Several different storage and archiving solutions are available from major vendors, differing in cost, technology, ease of access, and speed. A 3-Tbyte RAID storage unit is sufficient for keeping six months of records on-line for a typical hospital, and the prices are coming down, according to Oosterwijk. "Outsourcing is a viable option, using application service providers that charge for usage of the stored data."
TECHNOLOGY ISSUES"Getting patient information together with images is more of a challenge because of information standards. The Healthcare Level Seven Inc. (HL7) standard allows systems to talk to each other," says Mulvaney. "Many issues raised in handling sensitive medical data have already been solved in other industries. "A virtual private network (VPN) or encryption with various levels (of security) can avoid unauthorized access to patient information. The image isn't a problem unless it contains patient information. A bigger concern is inappropriate use of a PC in an authorized location. So a (part) of security is the auditing trail (to keep track of) who changes data."Says GE's Pearce, "We're not going to the Internet yet because we are not yet comfortable with security features. Over the next couple of years we should be able to deliver images and examination data over the Internet. For now the system is institution-based. But some customers are experimenting with VPNs."
Adds Pearson, "The biggest Web issue is the fact and perception of security. Ten years ago with all paper charts, the illusion was a 'solid bastion of security.' Now, our goal is to put the server on the Internet, so that eventually we can file and sign reports. As more information gets out there, how is it going to be used? Once the stuff is out in digital databases—and gets to insurers—who will ensure that it doesn't get around like a credit check?"
The National Electronic Manufacturers Association interface standard dealing with the digitization of medical images—Digital Image Communication—was developed jointly with the American College of Radiology to facilitate interoperability of medical equipment used in Picture Archiving and Communications Systems (PACSs). A PACS aims at connecting imaging devices, or modalities, and other compatible peripherals with workstations, storage devices, and servers.
Rapidly advancing technology is a concern for some users as it may affect long-term access to storage media and playback equipment. For example, "Optical jukeboxes are still around, but some users are concerned about early obsolescence," says Oosterwijk.
Dynamic Healthcare's Mulvaney says, "Image compression is okay using JPEG, which became part of DICOM. Wavelet compression is better and works well on radiology. The technology limitations of three to four years ago are largely solved now."
"There are no current provisions to provide DICOM over the Internet but the need exists, including security," says Henry Ford Health's Flynn. "We don't know how to deal with the DICOM exchange requirement that a device contacted knows the IP address of the initiator of the contact. Dynamic assignment of IP addresses through ISPs makes it almost impossible to identify a home user, for example."
GE Medical's Eric Pearce says, "We're developing an application-specific strategy, starting to connect, and looking at ways to integrate (our standard workstations) in the front end. The goal is to reduce customer cost and avoid obsolescence. We like seeing how we can merge technologies."
STANDARDS ORGANIZATIONSProfessional and trade associations are continuing to address standards for integration of PACS with hospital information systems (HIS) and radiological information systems (RIS) and to deal with issues such as expanded Internet access, tightened security, and remote storage of archived data. And legislation is pending regarding the confidentiality of patient information, under the Health Insurance Portability and Accountability Act, which will affect decisions about information system design.Since 1998, the Radiological Society of North America (RSNA; www.rsna) and the Healthcare Information and Management Systems Society (HIMSS; www.himss.org) have undertaken a joint effort to coordinate with the HL7 standard for hospital information systems. This effort is an industry initiative called "Integrating the Healthcare Enterprise (IHE; www.rsna.org/ihe)," whose objective is to bring the DICOM-based PACS, RIS, and HIS all closer to the HL7 standard.
Company InformationAgfaWilmington, MA 01887Web: www.agfa.comAmerican College of Radiology
Reston, VA 20191
Web: www.acr.org
Applicare Medical Imaging BV
3700 AX Ziest, The Netherlands
Web: www.applicare.com
Cedara Software Corp.
Mississauga, Ont., Canada L4N 1S7
Web: www.cedara.com
Dynamic Healthcare Technologies
Lake Mary, FL 32746
Web: www.dht.com
GE Medical Systems
Waukesha, WI 53188
Web: www.gemedicalsystems.com
Henry Ford Health System
Detroit, MI 48215
Web: www.henryfordhealth.org
National Electronic Manufacturers Association
Rosslyn, VA 22209
Web: www.nema.org
Oregon Health Sciences University
Portland, OR 97201
Web: www.ohsu.edu
Otech Inc.
Aubrey, TX 76227
Web: www.otechimg.com
Philips Medical Systems
Shelton, CT 06484
Web: www.medical.philips.com
Siemens Medical Systems
Concord, CA 94520
Web: www.siemens.com